Definition
ADH (antidiuretic hormone), also called vasopressin, is a peptide hormone produced by the hypothalamus and released by the neurohypophysis. It primarily regulates the body’s water balance by modulating water reabsorption in the kidneys. ADH acts on the renal collecting ducts, increasing water permeability and concentrating urine when the body is dehydrated or blood pressure drops. It also contributes to vasoconstriction, helping regulate blood pressure. Its secretion is stimulated by high plasma osmolality, low blood volume, or certain hormonal and neural signals. Insufficient or excessive ADH production leads to fluid and electrolyte disorders, such as diabetes insipidus or the syndrome of inappropriate ADH secretion (SIADH). ADH is therefore essential for maintaining water homeostasis and cardiovascular stability.
Origin and Context of Use
ADH is synthesized in the supraoptic and paraventricular nuclei of the hypothalamus and stored in the neurohypophysis. Initially identified for its role in blood pressure regulation, it is now studied and used in medicine for disorders related to water retention or dehydration. Plasma ADH measurements help evaluate endocrine dysfunctions, particularly central diabetes insipidus or SIADH. Synthetic ADH is also administered in intensive care to stabilize blood pressure in shock states or certain digestive hemorrhages, reflecting its physiological role in vasoconstriction and water regulation.
How It Works
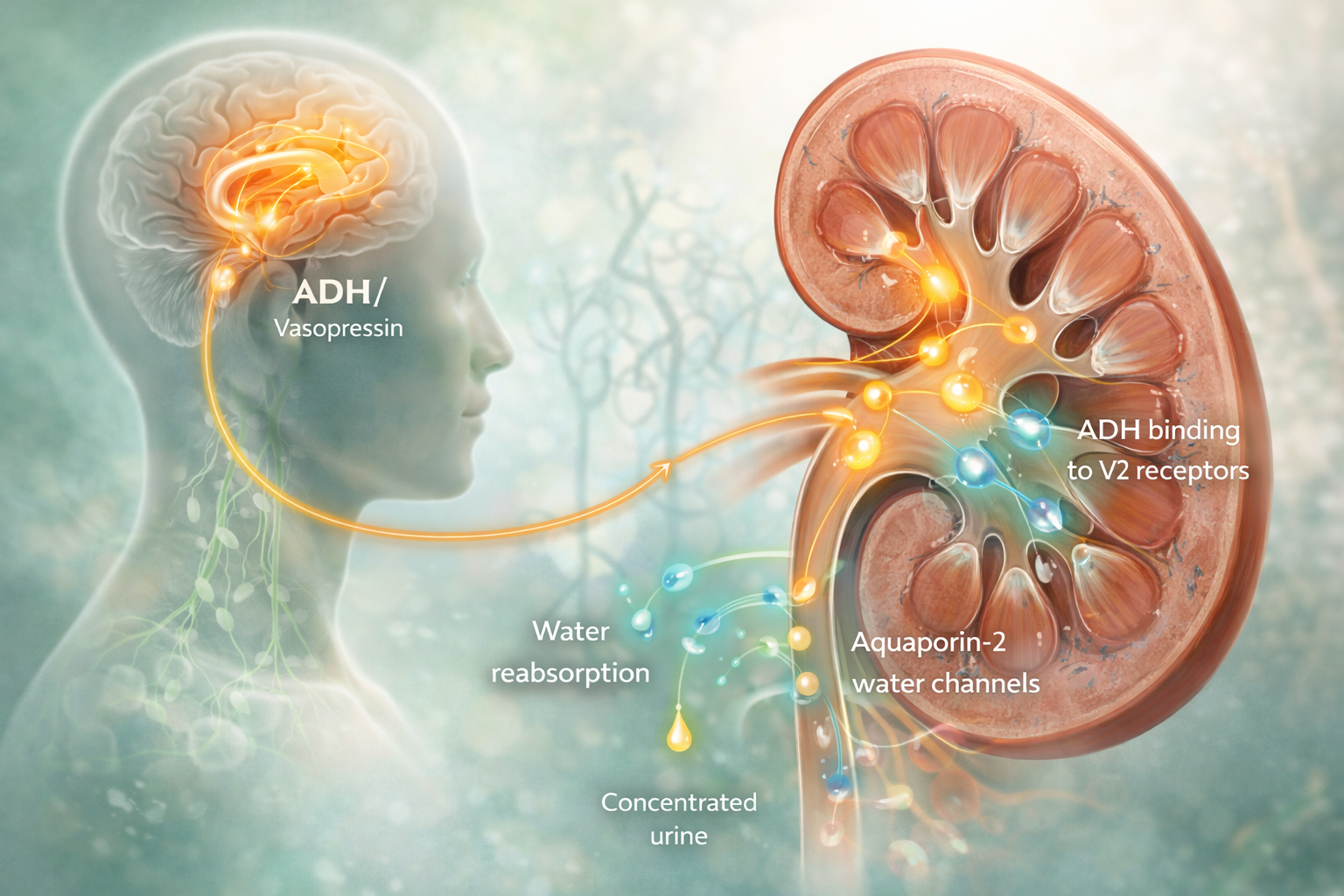
ADH binds to V2 receptors on cells of the renal collecting ducts. This triggers an intracellular cascade via cyclic AMP, causing the translocation of aquaporin-2 channels to the apical membrane, increasing water reabsorption into the bloodstream and concentrating urine. Vasopressin can also bind to V1 receptors on vascular smooth muscle cells, inducing vasoconstriction and raising blood pressure. ADH secretion is regulated by baroreceptors (sensitive to blood pressure) and osmoreceptors (sensitive to plasma osmolality). In hyperosmolar states, ADH increases to retain water; in hypoosmolarity or fluid overload, its secretion decreases. Non-osmotic factors such as pain, stress, or certain medications (corticosteroids, nicotine) also modulate ADH release, showing its complex adaptive role in maintaining homeostasis.
When It Is Used
Synthetic ADH or its analogues are used in several medical contexts: treatment of central diabetes insipidus, where the body does not produce enough ADH; management of SIADH to correct hyponatremia; stabilization of blood pressure during septic or hemorrhagic shock; treatment of certain digestive hemorrhages related to esophageal varices due to vasoconstrictive effects. It is also used in experimental protocols to monitor renal function and electrolyte balance.
Benefits and Goals
-
Maintain water balance and prevent dehydration.
-
Concentrate urine to prevent excessive water loss.
-
Stabilize blood pressure through vasoconstriction.
-
Correct hormonal disorders linked to diabetes insipidus or SIADH.
-
Facilitate medical control in shock or hemorrhagic states.
Risks, Limitations, or Controversies
Improper ADH administration can cause excessive water retention, severe hyponatremia, or cardiovascular complications. Patients with renal insufficiency or hypertension require close monitoring. Direct plasma ADH measurement is difficult, limiting precise evaluation of some disorders. Controversy exists over prolonged use of ADH analogues in intensive care due to the risk of tissue ischemia from excessive vasoconstriction.
Research and Innovations
Current research focuses on developing selective V2 receptor analogues to treat hyponatremia without vasoconstrictive effects and on identifying more reliable biomarkers for ADH to anticipate SIADH. Studies are also exploring ADH’s impact on the brain and cognition and its potential role in cardiovascular diseases. Engineering more stable, long-acting synthetic peptides improves pharmacokinetics for treating central diabetes insipidus and shock states.
Short FAQ
What is ADH?
ADH is an antidiuretic hormone that regulates water balance and blood pressure. It helps the body retain water when needed and contributes to vascular tone.
Where is it produced?
ADH is synthesized in the hypothalamus and stored in the neurohypophysis until released into the bloodstream.
How does it act on the kidneys?
It increases water permeability of the collecting ducts, allowing more water to be reabsorbed into the blood and concentrating the urine.
What are ADH receptors?
There are two main receptor types: V1 receptors on blood vessels, which mediate vasoconstriction, and V2 receptors on kidney cells, which regulate water reabsorption.
What happens if ADH is lacking?
A deficiency causes diabetes insipidus, characterized by excessive water loss and frequent, dilute urination.
What happens if ADH is excessive?
Excess ADH can lead to water retention and hyponatremia, potentially causing swelling, fatigue, and neurological symptoms.
Which factors influence its secretion?
Secretion is regulated by plasma osmolality, blood volume, stress, pain, and certain medications or hormonal signals.
What is synthetic ADH used for?
Synthetic ADH treats central diabetes insipidus, manages SIADH, and can stabilize blood pressure in certain critical care situations.
Can it affect blood pressure?
Yes. Through vasoconstriction, ADH can elevate blood pressure, particularly during states of low blood volume or shock.
How is ADH measured?
It can be measured directly in plasma or indirectly by assessing urine osmolality and water retention patterns.
Key Points
ADH is central for regulating body water and blood pressure. Its action on kidneys and vessels maintains hydric and cardiovascular homeostasis. Disorders of its production lead to specific pathologies, and synthetic analogues provide targeted therapeutic options with monitoring to prevent complications.
Related Longevity Concepts
Scientific context
Field: Clinical medicine, biology, and preventive health
Biological process: Human physiology, pathology, and health-related mechanisms
Related systems: Metabolic, immune, cardiovascular, nervous, and cellular systems
Relevance to longevity: Understanding medical terminology and biological processes helps clarify how diseases, symptoms, biomarkers, and treatments influence long-term health, prevention, and healthy aging.