Definition
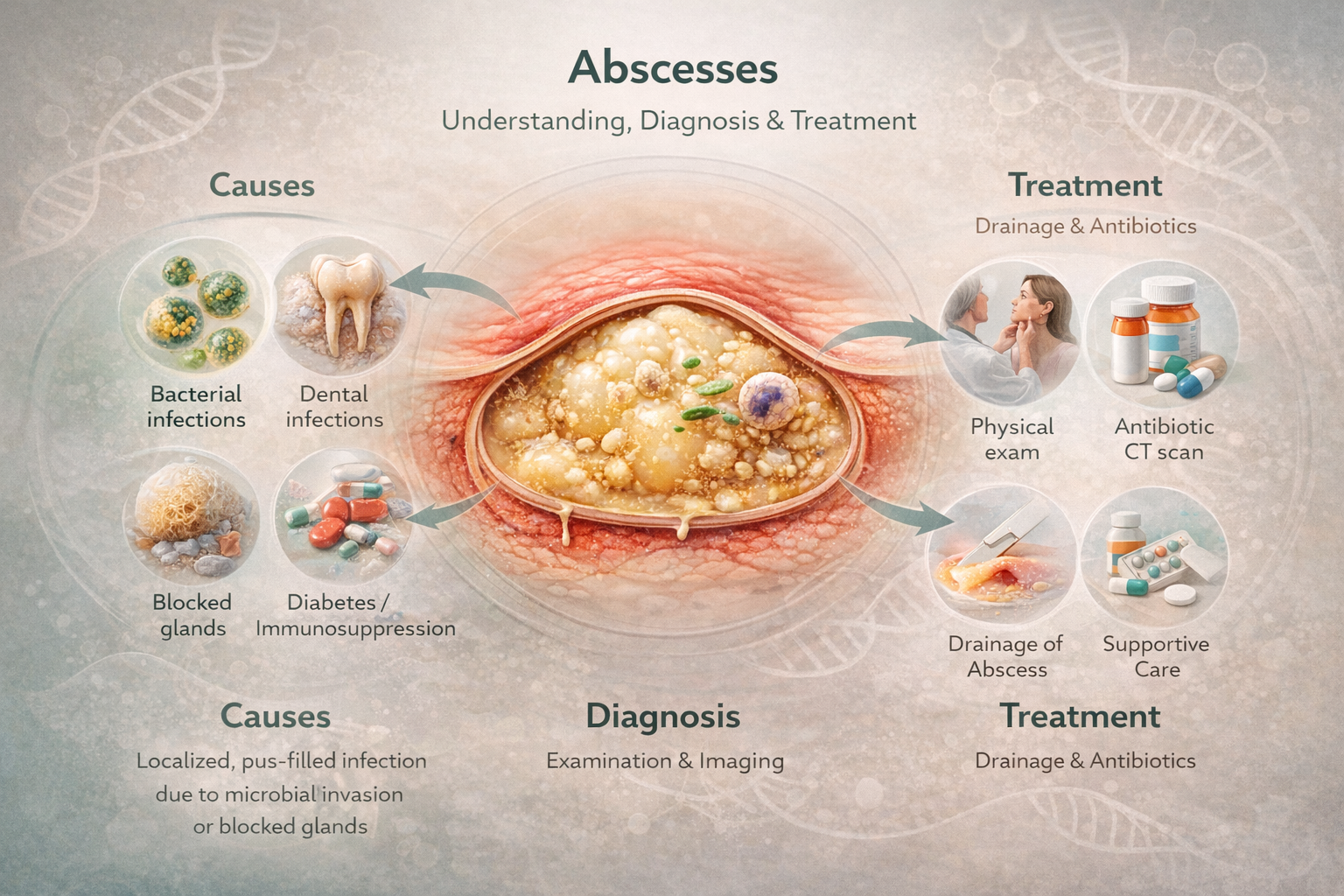
An abscess is a localized collection of pus within tissues, usually caused by a bacterial infection. It is characterized by inflammation, redness, pain, and warmth at the affected site. Pus consists of bacteria, dead immune cells, and tissue debris. Abscesses can develop in the skin, internal organs, or body cavities and vary in size, from a few millimeters to several centimeters. They represent a protective response of the body to isolate and contain the infection but can cause complications if bacterial spread continues. Superficial skin abscesses are visible, while internal abscesses require imaging for detection. The formation of an abscess indicates that the immune system is actively working to eliminate the infection and limit damage to surrounding tissues.
Origin and Context of Use
The term “abscess” comes from the Latin abscessus, meaning “a going away,” reflecting the process of separation of infected tissue. Abscesses occur in various medical contexts: skin infections, post-surgical sites, dental infections, or chronic diseases such as diabetes or inflammatory disorders. In clinical practice, rapid identification is essential to prevent infection spread. Skin abscesses are common in general practice, while internal abscesses, such as liver or brain abscesses, require hospital care. Their presence often signals a bacterial infection requiring targeted intervention, combining drainage and antibiotics depending on the location and severity. Epidemiological factors like immunosuppression or prolonged antibiotic use increase the risk of abscess formation.
How Does It Work?
Abscess formation begins when bacteria, typically Staphylococcus aureus or Streptococcus spp., invade tissue. The body triggers a local immune response: neutrophils and macrophages migrate to the infected site and release enzymes to destroy bacteria. This reaction causes partial tissue necrosis and accumulation of pus, forming the abscess core. A fibrous capsule develops around this cavity, isolating the infection and limiting its spread. This isolation explains the fluctuation in swelling and tenderness upon palpation. Internal abscesses can compromise organ function and cause systemic symptoms such as fever or malaise. Spontaneous or surgical drainage is often necessary to remove pus, complementing the immune response and preventing bacterial dissemination. Antibiotics target remaining bacteria but are usually insufficient alone for encapsulated abscesses.
When Is It Used?
Detection and treatment of abscesses are critical in several clinical situations:
-
Skin or subcutaneous abscesses causing localized pain and redness.
-
Dental or periapical abscesses causing infection and swelling in oral tissues.
-
Internal abscesses (liver, brain, lung) affecting organ function.
-
Post-operative or traumatic abscesses to prevent bacterial spread.
-
Immunocompromised patients to reduce the risk of sepsis.
Medical intervention depends on abscess size, location, severity, and the patient’s general condition.
Benefits and Objectives
Treating an abscess aims to:
-
✔ Eliminate the source of infection.
-
✔ Prevent bacterial spread and sepsis.
-
✔ Relieve pain and inflammation.
-
✔ Promote rapid healing and limit sequelae.
Proper drainage combined with targeted antibiotics ensures complete resolution while minimizing the risk of recurrence.
Risks, Limits, or Controversies
Abscesses may lead to complications if treatment is delayed: spontaneous rupture, infection spreading into the bloodstream, or damage to neighboring organs. Antibiotics alone are often insufficient for encapsulated abscesses, necessitating drainage. Deep abscesses may require complex surgical intervention. In immunocompromised patients, healing is slower and recurrences are more frequent. There is also debate about the systematic use of antibiotics after drainage of a small skin abscess, with studies suggesting drainage alone may suffice.
Research and Innovations
Current research explores less invasive image-guided drainage, antibacterial biomaterials to reduce recurrence, and rapid pathogen identification using molecular tests. Studies also evaluate new antibiotics and monoclonal antibodies targeting Staphylococcus aureus. Telemedicine and wearable sensors are being tested to detect early inflammation and monitor skin abscesses at home. The goal is to reduce complications, surgical interventions, and hospitalization duration while personalizing treatment according to bacterial and immune profiles.
Short FAQ
What is an abscess?
An abscess is a collection of pus in tissue or an organ caused by a bacterial infection.
What are the symptoms?
Pain, redness, warmth, swelling, and sometimes fever.
How does an abscess form?
Bacteria trigger a local immune response, leading to pus accumulation and capsule formation.
Is drainage always necessary?
Yes, drainage is often required to remove pus and complement antibiotics.
Which antibiotics are used?
Treatment targets mainly Staphylococcus aureus and depends on susceptibility testing.
Can an abscess go away on its own?
Small superficial abscesses may resolve, but most require medical intervention.
What are the risks if untreated?
Infection spread, sepsis, organ damage, or recurrence.
How to prevent skin abscesses?
Maintain local hygiene, promptly treat wounds, and address early infections.
Can multiple abscesses occur simultaneously?
Yes, especially in immunocompromised patients or those with chronic diseases.
Which tests detect internal abscesses?
Ultrasound, CT scan, MRI, or blood tests depending on location.
Key Points
An abscess is the body’s response to isolate a bacterial infection. Drainage and antibiotics are essential to prevent spread and ensure healing. Location and size determine treatment strategy. Early detection reduces complications and supports recovery.
Related Longevity Concepts
Scientific context
Field: Clinical medicine, biology, and preventive health
Biological process: Human physiology, pathology, and health-related mechanisms
Related systems: Metabolic, immune, cardiovascular, nervous, and cellular systems
Relevance to longevity: Understanding medical terminology and biological processes helps clarify how diseases, symptoms, biomarkers, and treatments influence long-term health, prevention, and healthy aging.