Definition
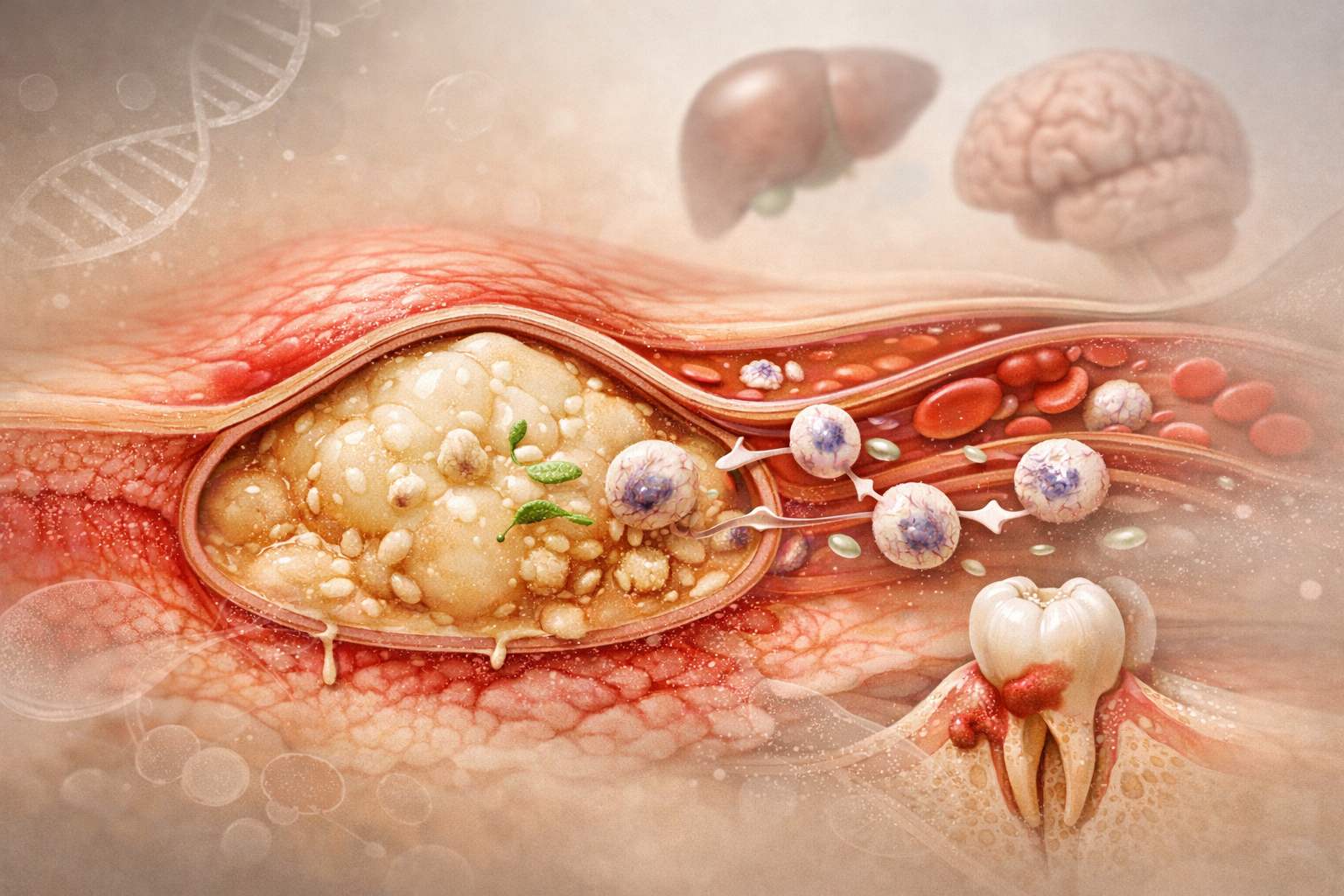
An abscess is a localized accumulation of pus within a body tissue. This purulent collection most often results from a bacterial infection and reflects a defensive response of the immune system aimed at isolating the infectious agent. The pus contained in an abscess is composed of bacteria, dead or active white blood cells, cellular debris and inflammatory fluid.
An abscess may develop in different tissues, including the skin, teeth, gums, internal organs or deeper tissues. When superficial, it usually appears as a painful swelling that is red and warm to the touch. When located deeper in the body, symptoms may include fever, localized pain or signs related to the affected organ.
The formation of an abscess represents an attempt by the body to limit the spread of infection. An inflammatory membrane forms around the infected area, creating a closed cavity that contains the pus. Without appropriate treatment, this accumulation may increase in size, rupture spontaneously or lead to local or systemic complications.
Origin and context of use
The term “abscess” comes from the Latin word “abscessus”, meaning “a going away” or “separation”. Historically, the term reflected the idea that harmful bodily substances withdrew into a cavity in the body. This concept dates back to ancient medical traditions, particularly Hippocratic medicine.
Knowledge about abscesses evolved with the development of microbiology in the nineteenth century. The work of Louis Pasteur and Robert Koch helped demonstrate the role of bacteria in the development of purulent infections. Abscesses are now understood as a localized immune response to microbial invasion.
The term is used in many medical disciplines including dermatology, surgery, dentistry, infectious disease medicine and radiology. Several types of abscesses are distinguished according to their location, such as cutaneous abscesses, dental abscesses, lung abscesses, brain abscesses or intra-abdominal abscesses. Each type involves specific clinical mechanisms and implications.
How does it work?
Abscess formation generally begins with the introduction of microorganisms into a tissue. This may occur after a wound, obstruction of a hair follicle, dental infection, surgical procedure or spread from an existing infection.
When bacteria invade the tissue, the immune system triggers an inflammatory response. White blood cells, particularly neutrophils, migrate to the infected site to destroy the pathogens. This process leads to the accumulation of immune cells, bacteria and damaged tissue components.
This accumulation progressively forms pus. The surrounding tissue reacts by creating an inflammatory capsule composed of fibers and immune cells. This capsule limits the spread of infection to nearby tissues.
Pressure inside the cavity increases as pus accumulates. This pressure explains the pain often associated with an abscess. When the abscess is superficial, it may open spontaneously and drain its contents. In other situations, a medical procedure is required to evacuate the pus and treat the infection.
Without drainage or appropriate antibiotic therapy, the infection may spread and potentially lead to systemic infection such as sepsis.
In which situations is it used?
The term abscess is used to describe several clinical situations involving a localized infection. It frequently appears in the diagnosis of dermatological or dental conditions.
Cutaneous abscesses often occur following infection of a hair follicle, contamination of a wound or obstruction of a skin gland. They commonly appear in areas such as the armpits, buttocks or face.
Dental abscesses develop when bacteria infect the dental pulp or tissues surrounding the tooth. They may cause intense pain and swelling of the gums.
Internal abscesses affect organs such as the liver, lungs or brain. Their diagnosis often relies on medical imaging techniques including ultrasound, computed tomography or magnetic resonance imaging.
In all cases, identification and drainage of the purulent collection remain central to treatment.
Benefits and objectives
The formation of an abscess represents a physiological defense mechanism that helps confine an infection to a limited area of tissue.
Biological and clinical objectives include:
✓ Isolating bacteria to prevent their spread within the body
✓ Concentrating immune cells at the infection site
✓ Limiting damage to surrounding tissues
✓ Allowing elimination of pus through natural or medical drainage
✓ Facilitating healing once the underlying infection is treated
This containment mechanism may sometimes prevent a generalized infection. In clinical practice, early recognition of an abscess allows targeted treatment combining drainage and, when necessary, antibiotic therapy.
Risks, limits or controversies
An untreated abscess can lead to several complications. Progressive enlargement of the purulent collection may damage surrounding tissues or compress important anatomical structures.
Spontaneous rupture of an abscess may allow bacteria to spread to nearby tissues or into the bloodstream. In some cases, this dissemination may result in sepsis, a potentially severe systemic infection.
Deep abscesses may be difficult to diagnose because symptoms are sometimes nonspecific. Medical imaging is therefore essential to locate the purulent collection.
Certain antibiotic-resistant bacteria, such as methicillin-resistant Staphylococcus aureus, can complicate management and require specific treatment strategies.
Research and innovations
Current research focuses on improving the diagnosis and treatment of abscesses, particularly those located deep in the body or difficult to access.
Advances in medical imaging allow more precise detection of purulent collections. Ultrasound-guided and CT-guided drainage techniques now enable minimally invasive procedures that reduce the need for traditional surgery.
Molecular microbiology techniques also allow faster identification of the bacteria responsible for infection and help guide appropriate antibiotic therapy.
Research is also exploring interactions between bacteria and the immune system during pus formation. These studies aim to better understand the inflammatory mechanisms involved and support the development of more targeted therapeutic strategies.
Short FAQ
What is the pus contained in an abscess?
Pus is a thick fluid composed of white blood cells, bacteria, cellular debris and inflammatory proteins. It forms when the immune system reacts to a localized infection within a tissue.
Can an abscess disappear without treatment?
Small superficial abscesses may sometimes drain spontaneously and heal. Larger abscesses usually require medical drainage in order to remove the pus and prevent complications.
Which bacteria most often cause abscesses?
Bacteria of the genus Staphylococcus, particularly Staphylococcus aureus, are frequently involved. Other bacteria may be responsible depending on the location of the infection.
How can a cutaneous abscess be recognized?
A cutaneous abscess usually appears as a swollen, red, warm and painful lump. A softer central area may indicate the presence of pus beneath the skin.
Why are abscesses painful?
Pain results from the pressure created by the accumulation of pus inside the cavity and from inflammation of the surrounding tissues.
Is an abscess contagious?
The abscess itself is not contagious. However, some bacteria present in the pus may be transmitted through direct contact with infected material.
What is the main treatment for an abscess?
Treatment usually involves draining the pus, a procedure performed by a healthcare professional. Antibiotics may also be prescribed depending on severity and location.
Can an abscess form in internal organs?
Yes. Abscesses may develop in organs such as the liver, lungs, brain or abdomen. They are generally detected using medical imaging techniques.
How long does an abscess take to heal?
Healing time depends on the size, location and treatment. After drainage and appropriate management, most abscesses heal within several days to a few weeks.
Can abscess formation be prevented?
Proper wound hygiene, early treatment of infections and regular dental care help reduce the risk of abscess formation.
Key points
An abscess is a localized accumulation of pus caused by a bacterial infection. This reaction represents an attempt by the immune system to confine microorganisms and limit their spread. Abscesses can form in the skin, teeth or internal organs. Diagnosis relies on clinical examination and sometimes medical imaging. The main treatment consists of draining the purulent collection and addressing the underlying infection. Without appropriate management, infectious complications may occur.
Related Longevity Concepts
Scientific context
Field: Clinical medicine, biology, and preventive health
Biological process: Human physiology, pathology, and health-related mechanisms
Related systems: Metabolic, immune, cardiovascular, nervous, and cellular systems
Relevance to longevity: Understanding medical terminology and biological processes helps clarify how diseases, symptoms, biomarkers, and treatments influence long-term health, prevention, and healthy aging.