Definition
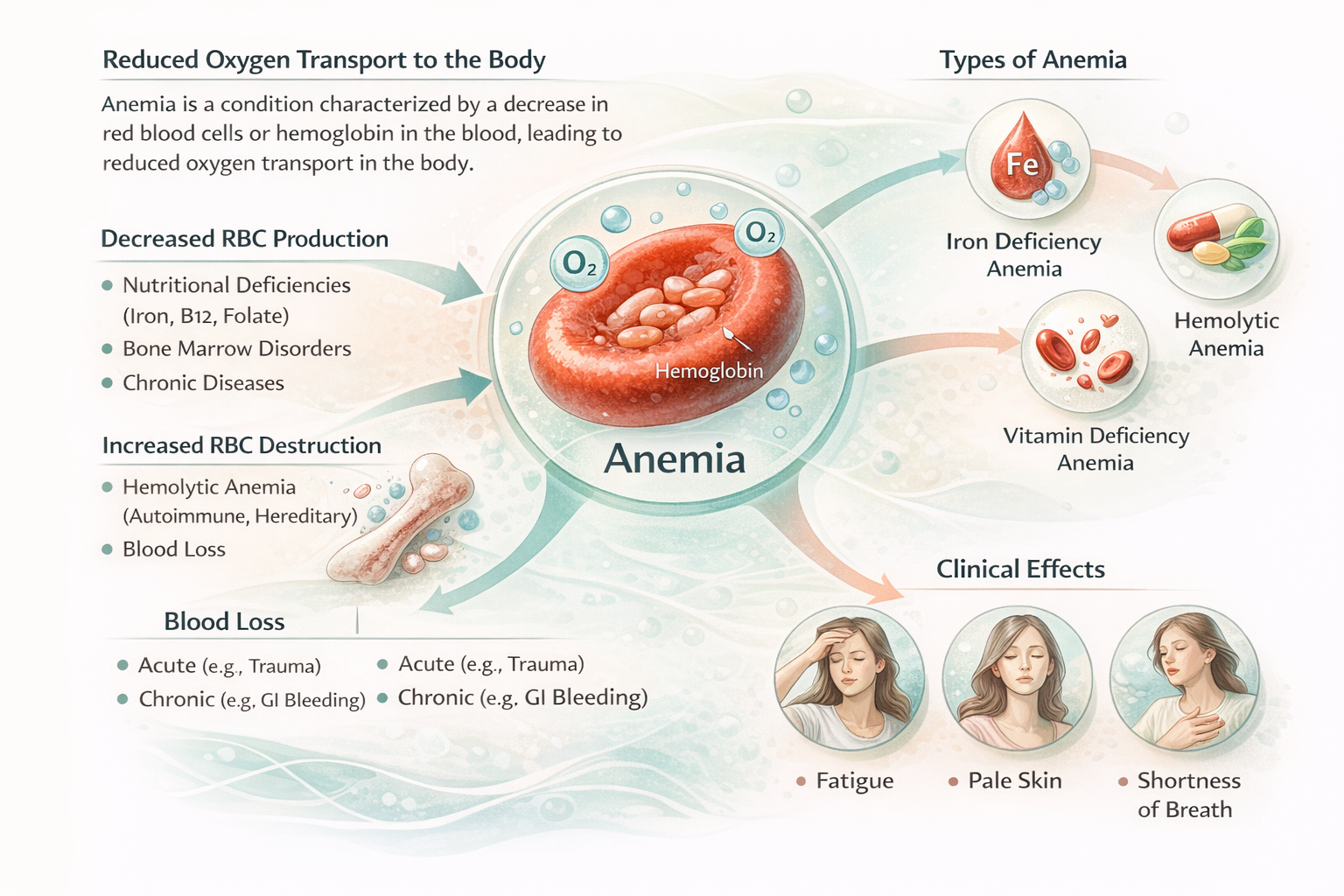
Anemia refers to a reduction in hemoglobin concentration in the blood or in the number of circulating red blood cells. Hemoglobin, a protein found in red blood cells, transports oxygen from the lungs to tissues. When its level is insufficient, the body receives less oxygen, causing fatigue, pallor, shortness of breath, and sometimes palpitations. Diagnostic thresholds vary by age, sex, and pregnancy, but hemoglobin below 13 g/dL in adult men and 12 g/dL in adult women is generally considered abnormal. Anemia can be acute or chronic and results from different mechanisms: insufficient red blood cell production, accelerated destruction (hemolysis), or blood loss. It may occur alone or alongside other blood disorders, and identification often requires a complete blood analysis, including a complete blood count, ferritin, vitamin B12, and folate levels.
Origin and context of use
The term “anemia” comes from the Greek word “anaimia,” meaning “lack of blood.” It has been studied since antiquity, but modern understanding relies on physiology and hematology. Clinically, anemia is a key indicator of underlying conditions such as nutritional deficiencies, chronic diseases, hematologic disorders, or acute blood loss. It is commonly encountered in general medicine, pediatrics, geriatrics, and obstetric care. Early recognition helps prevent complications related to tissue hypoxia and guides targeted management, whether supplementation, transfusion, or treatment of the underlying disease.
How it works
The body produces red blood cells in the bone marrow from stem cells, a process regulated by erythropoietin, a hormone produced by the kidneys. Red blood cells contain hemoglobin, which binds oxygen in the lungs and releases it to tissues. Anemia can occur when:
-
red blood cell production is insufficient (iron, vitamin B12, folate deficiencies, bone marrow failure);
-
red blood cell destruction is excessive (autoimmune hemolysis, membrane or enzyme defects);
-
there is acute or chronic blood loss (trauma, heavy menstruation, digestive ulcers).
The body compensates by increasing heart rate, breathing, and tissue oxygen extraction. Clinical signs depend on the severity and speed of anemia onset: rapid drop causes intense fatigue and dizziness, whereas chronic anemia may remain asymptomatic until advanced stages.
When it is used
Anemia diagnosis applies in several contexts:
-
screening during routine or preoperative exams;
-
monitoring chronic diseases such as kidney failure, liver disease, or inflammatory conditions;
-
surveillance of at-risk populations: pregnant women, infants, elderly;
-
investigating unexplained fatigue, pallor, or shortness of breath;
-
guiding therapy for iron, vitamin B12, folate supplementation, or transfusion.
Benefits and objectives
Management of anemia aims to:
-
restore normal hemoglobin levels;
-
improve oxygen transport to tissues;
-
reduce fatigue and shortness of breath;
-
prevent cardiac or neurological complications;
-
address the underlying cause, whether deficiency, hemorrhage, or bone marrow disorder.
Risks, limitations, or controversies
Anemia management has limitations:
-
iron supplements can cause constipation, abdominal pain, and overdose;
-
blood transfusions carry risks of allergy or infection;
-
some genetic or autoimmune anemias remain difficult to treat;
-
diagnosis may be delayed with atypical or mild symptoms, postponing management.
Research and innovations
Current research focuses on:
-
identifying early biomarkers for anemia before symptoms appear;
-
developing targeted therapies for genetic anemias such as beta-thalassemia or sickle cell disease;
-
improving iron supplement formulations to reduce side effects;
-
using recombinant erythropoietin and new molecules stimulating red blood cell production;
-
non-invasive techniques to measure hemoglobin and tissue oxygenation.
Short FAQ
What is anemia?
A reduction in hemoglobin or red blood cells, decreasing oxygen delivery to tissues.
What are the main symptoms?
Fatigue, pallor, shortness of breath, palpitations, and dizziness.
How is anemia diagnosed?
Through blood tests, complete blood count, ferritin, vitamin B12, and folate levels.
What are the types of anemia?
Iron deficiency, megaloblastic, hemolytic, aplastic, or anemia related to chronic disease.
Can anemia be serious?
Yes, especially if severe or rapid, leading to tissue hypoxia and cardiac complications.
How is iron-deficiency anemia treated?
Iron supplements, dietary adjustments, and treatment of the underlying deficiency.
Is anemia hereditary?
Some forms, like thalassemia or sickle cell disease, are inherited.
Can anemia be prevented?
Adequate intake of iron, vitamin B12, folates, and medical monitoring for at-risk populations.
Does pregnancy increase anemia risk?
Yes, due to higher demands for iron and red blood cells.
Is transfusion always necessary?
No, it depends on anemia severity and underlying cause.
Key points
Anemia reflects insufficient hemoglobin or red blood cells, leading to tissue hypoxia. Detection relies on blood tests and biochemical assays. Causes include deficiencies, blood loss, or genetic disorders. Management aims to correct the cause, restore oxygenation, and prevent complications.
Related Longevity Concepts
Scientific context
Field: Clinical medicine, biology, and preventive health
Biological process: Human physiology, pathology, and health-related mechanisms
Related systems: Metabolic, immune, cardiovascular, nervous, and cellular systems
Relevance to longevity: Understanding medical terminology and biological processes helps clarify how diseases, symptoms, biomarkers, and treatments influence long-term health, prevention, and healthy aging.

